- Austausch & Vernetzung
- Wissen & Lernen
- Advocacy
- Unsere Themen
Von Carine Weiss
Palliative care and pain relief are among the most neglected dimensions of global health today, not least in discussions around universal health coverage. Scientific and medical advances in the last century have prolonged and facilitated life and delayed death. The increasing prevalence of non-communicable diseases and aging populations mean that the demand for palliative care and medicine will continue to grow worldwide.
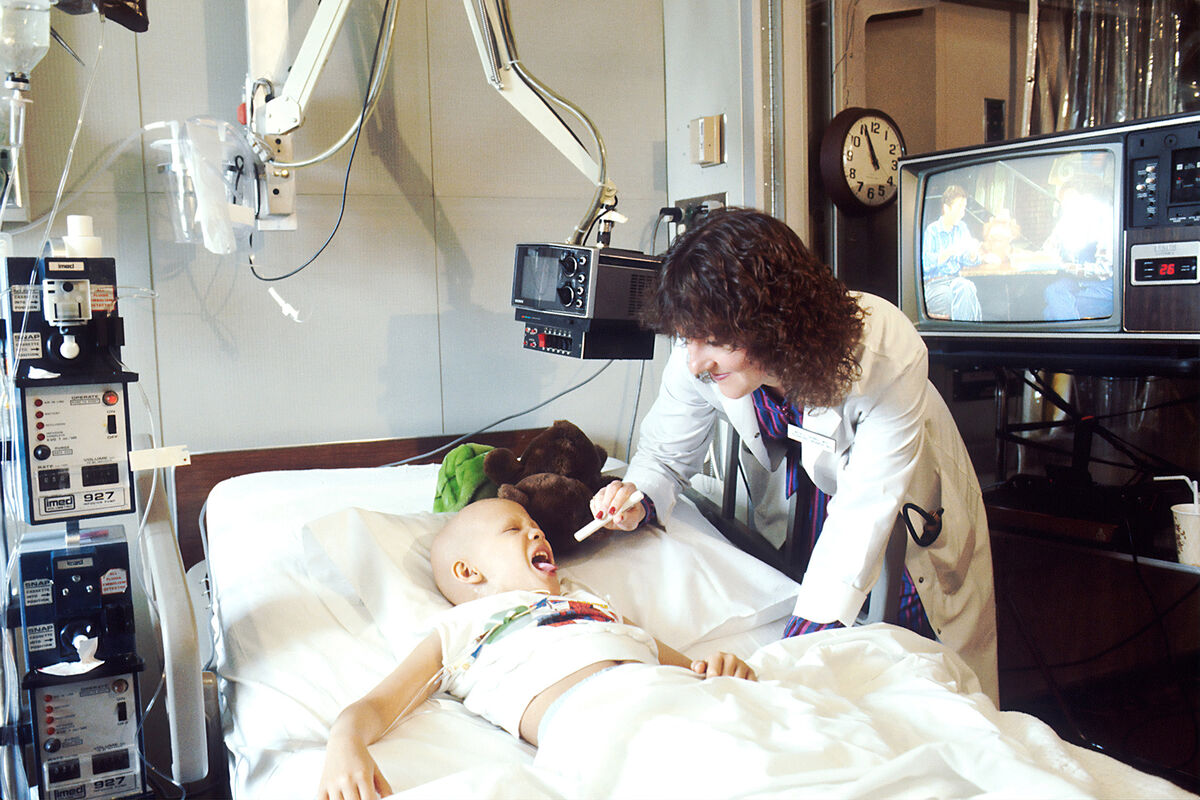
In 2018, around 18.1 million new cases of cancer were diagnosed globally (WHO, 2018a). Low and middle-income countries (LMIC) are experiencing an increase in the burden of non-communicable diseases, including cancer. By 2035, about two-thirds of new cancer cases will be diagnosed in LMICs and this will further challenge their already weak healthcare systems (Abu-Odah, Molassiotis and Liu, 2020).
Palliative care is a human right, and yet there are significant disparities in its provision across the globe. Each year, an estimated 40 million people require palliative care, 78% of whom live in low and middle-income countries. But around the world, only approximately 14% of people who need palliative care are currently receiving it (WHO, 2018b; Clark et al., 2020).
In 2014, the World Health Assembly passed a resolution (World Health Assembly resolution WHA67.19) urging governments to integrate palliative care into their existing healthcare services (WHO 2014; Carrasco et al. 2020). The WHO recommends that palliative care becomes an integral part of healthcare and that all patients affected by a life-threatening disease should have access to such services. However, it is unclear which models best fit individual countries and their health systems.
Palliative care (PC) refers to all the services provided to make the remaining life of a terminally ill patient meaningful and valuable. According to the WHO definition, “palliative care is an approach that improves the quality of life of patients and their families facing the problem associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual” (WHO 2002; WHO 2018c).
One of the strengths of palliative care is its recognition of the human side of an illness. For example, cancer patients in need of palliative care are a group of people with high psychosocial, spiritual and physical needs who experience many different symptoms, especially connected to pain. In short, palliative care is a philosophy of care based on a holistic approach to care and support for patients and their families, including in the mourning period.
The goal of palliative care is to restore the functional capacity of a patient. It does this by being sensitive to the cultural and local values, beliefs and practices of an individual in order to alleviate pain and improve their quality of life by controlling their symptoms once a disease can no longer be cured.
The development of palliative care follows a public health model drawn up by the WHO that emphasises health policy, education, availability of medication and implementation (WHO, 2018c; Callaway, 2018). There are many barriers to achieving each of these components.
Without policies for clinical guidelines, national standards of care, and laws or regulations governing the providers which support the provision of palliative care, it is challenging to establish any model for this type of care. As LMICs witness a sharp growth in the burden of non-communicable diseases such as cancer, there is a significant gap between the demand for and supply of palliative care in these countries.

A systematic review of reviews has revealed that the development of a palliative care model for cancer patients is being made more difficult by the limited understanding of what this type of care actually is, the low number of staff trained in such care, insufficient drug supply and a lack of comprehensive national plans for its implementation (Abu-Odah, Molassiotis and Liu, 2020).
Fragile health systems lack the safety nets of health insurance schemes, social support programmes and, critically, palliative care services, for patients with incurable diseases. This results in the very high costs of care being, by necessity, absorbed by the individual, their families and the local community. Direct costs involve medical expenses including medication, treatments and travel costs to and from a health centre. Indirect costs, such as taking time off work or school, are less visible but they nevertheless place a huge financial burden on families who are unable to save any money for the future. The costs of illness are far less well understood in LMICs in comparison to the relatively well-functioning palliative care services in the West. When assessing the costs of ill health, palliative care can be defined as a poverty-reduction strategy (Anderson & Grant, 2017).
One reason why palliative care models have been neglected so far is that this type of care is often considered to be a luxury that it would be nice for healthcare systems to have, but which is not essential. Even high-income countries with well-functioning health systems struggle to provide access to comprehensive palliative care programmes (Horton, 2018).
To foster the development of palliative care, we must understand the challenges on every level, including health policy, education, availability of medication and implementation. We must then act on this knowledge by bringing together clinicians, patients and their families and policy makers. Palliative care requires a multidisciplinary team approach comprising professionals working towards a common goal. No single model is suitable for all conditions. However, there is a universal fundamental principle of palliative care: it should address the individual wishes and needs of each patient and their relatives.
Modelling exercises on non-communicable diseases reveal that their incidence rate is set to increase steadily during the coming decades. Palliative care is a human right. It must be fully integrated into universal health coverage if we want to mitigate against a catastrophic weakening of health systems and to alleviate the suffering of millions of patients and their families (Seelemann et al. 2019)
This Bulletin is dedicated to shedding light on the current situation of palliative care around the world.